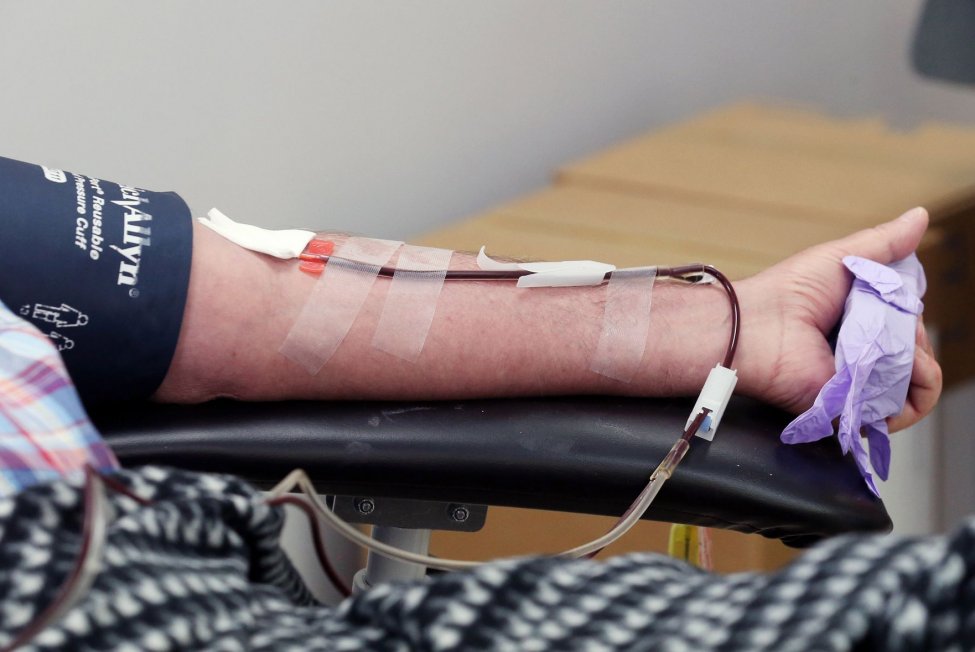
Jan. 25 (UPI) — Using blood plasma collected from patients who have recovered from COVID-19 to treat those actively battling the virus only works in some cases, an analysis published Tuesday by JAMA Network Open found.
Only a “narrow window” exists in which the treatment, which relies on the plasma from recovered patients that contains antibodies against the virus “might be effective,” the researchers said.
That window includes patients sick enough to require hospitalization, but who have not yet developed illness severe enough to require treatment in the intensive care unit or mechanical ventilation to maintain their breathing, they said.
“Our study showed that while convalescent plasma did not have a strong beneficial effect on average, there were subgroups of patients in whom the therapy appeared to help,” study co-author Andrea B. Troxel told UPI in an email.
“These were patients with the least severe disease, and with other pre-existing conditions such as diabetes, [heart] disease and [lung] disease,” said Troxel, a professor of population health at New York University in New York City.
Convalescent plasma has been used as a treatment for infectious diseases for more than a century, according to the National Institutes of Health. Blood is collected from patients who have recovered from infection and transfused into those actively battling it, with the goal of boosting their antibody levels, the agency says.
Antibodies are proteins produced by the immune system to fight off infections.
Although the NIH last year halted a large clinical trial of convalescent plasma in treating COVID-19, due to a lack of clinical benefit, several studies since have found it can be effective, if used correctly.
Still, the World Health Organization continues to recommend against using convalescent plasma in most cases.
For best result, the plasma, which is administered via transfusion, must be initiated early in the course of the disease, in hospitalized patients, before they require high levels of supplemental oxygen or become hypoxic, or oxygen deprived, these studies found.
Additional research has shown that convalescent plasma transfusion can reduce the risk for hospitalization in patients who receive it within seven days of diagnosis.
Troxel and her colleagues analyzed data from eight studies of convalescent plasma therapy that collectively enrolled 2,369 participants.
Across all of the included studies, the treatment boosted odds of recovery from COVID-19 among hospitalized patients by 6%, the data showed.
However, the odds were better for those administered the treatment earlier in their hospitalizations and those with less serious illness as defined by the WHO’s symptoms severity scale, the researchers said.
“Because [our] study was so large and the methods so rigorous, we were able to show that while convalescent plasma doesn’t benefit all patients, it may have positive effects in certain subgroups,” Troxel said.
“If patients are already hospitalized and severely ill, as in our study, it may be too late for convalescent plasma to work.”